Welcome to the Transforming Perceptions of Nursing and Midwifery 30 Day Challenge for December 2018!
“Mentor a junior colleague or student or reverse mentor a senior nurse or midwife."

These Ten Top Tips for Mentoring and Reverse Mentoring detail what makes a great mentor and reverse mentor, as well what makes a less good one. The tips have been co-created with nursing and midwifery ambassadors from acute and primary care; a variety of specialties and those with different portfolios.
What Is Mentoring?
Mentoring is a long standing and increasingly popular tool for supporting personal development.
Traditionally, mentoring is the long term passing on of support, guidance and (sometimes) advice. In the workplace it has tended to describe a relationship in which a more experienced colleague uses their greater knowledge and understanding of the work or workplace to support a more junior or inexperienced member of staff. Sometimes a more junior member of staff may have greater knowledge or experience in certain aspects of work or the workplace and they may act as the mentor. Mentoring can also take place peer-in-peer relationships.
In summary:
- Mentoring should be driven by the person being mentored.
- It is essentially a supportive form of development.
- It focuses on helping an individual manage their career and improve skills.
- Personal issues can be discussed more productively unlike in coaching where the emphasis is on performance at work.
- Mentoring activities have both organisational and individual goals.
There is often confusion about how mentoring differs from coaching. Coaching is about developing a person’s skills and knowledge in order to help them increase and improve their performance and contribute to fulfilling an organisation’s objectives. The aim is to focus on specific skills and goals. Coaching is usually a more formal relationship than mentoring.
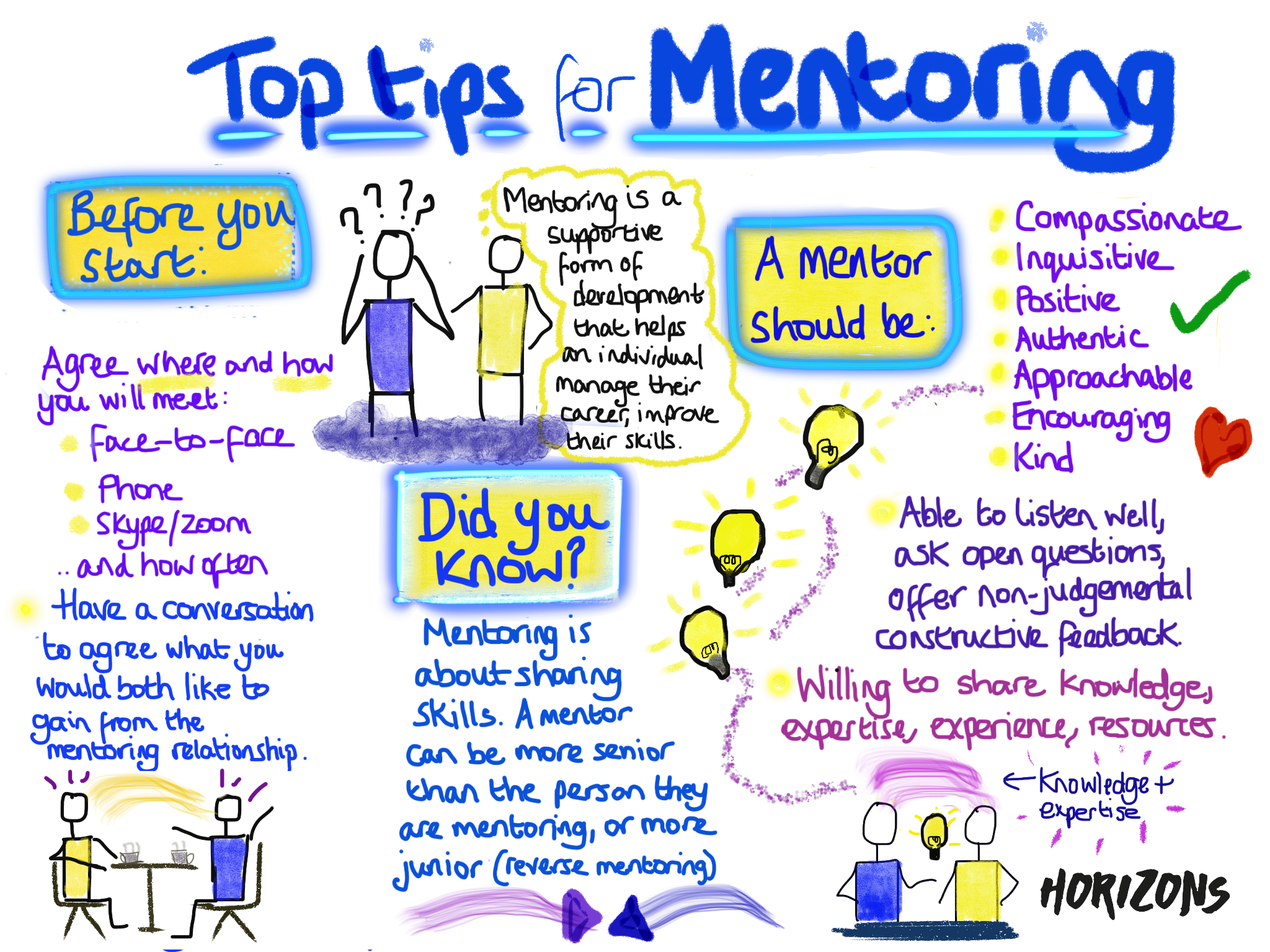
Mentoring Ten Top Tips
These top 10 tips are for both Mentors and Mentees to consider:
Top Tip 1: Reverse mentoring
Traditional mentoring has usually stressed that the mentor is more senior (and often older) than the mentee. In our environment, mentoring can be peer-to-peer, or the mentor can be a younger or junior person who has the skills and knowledge that someone older or more senior might find helpful. One example is that many younger people in the workplace are more skilled at understanding and working with digital platforms and using computers.
Staff can mentor others who do not have certain skills, e.g. some nurses have greater experience in certain clinical areas and some have more experience of management skills. Management is something that people often take on because of their clinical skills and experience but it may require a different mind-set as well as learning new skills.
Reverse mentoring can be organised i.e. you can arrange meetings at a specific time or it might be more spontaneous, at a time when someone needs support on the spot.
Top Tip 2: Have a clear contract
At the start of the relationship, take the time to discuss what both parties expect. This is known as a ‘contract’. In the contract it’s useful to cover mutual expectations: what each of you want from the session(s) and how you might want to go about learning together; and boundaries like confidentiality. The contract does not always need to be in writing but it needs to be discussed and agreed at the outset to make the arrangement clear.
Also think about how you will define success in your mentoring relationship. What will good look like? How will you evidence success? This needn’t be an onerous process: asking for one thing the mentee got out of the session, a one to ten scale or even using an emoji of some sort to express a view can sometimes be a simple and powerful way of measuring impact.
It’s useful to remember that the relationship should be led by the mentee – it’s about building their skills and confidence so they need to be proactive, and responsible for actions that are personal and relevant to them as an individual.
Sometimes a person has a coach as well as mentor. If this is the case, when setting your contract it will be useful for you to bear this in mind.
Top Tip 3: Take action if mentoring isn’t working for you
You need to know what you do if your mentor isn’t the one for you, if you don’t get on or you don’t feel that you are getting what you need through the relationship. It is important to recognise that not all relationships work well that doesn’t necessarily imply blame on either party. Sometimes there’s just not rapport – you don’t ‘gel’.
Being clear about your own needs as well as identifying and expressing what is not working for you is key. It is vital that you feel sufficiently confident to say positively and powerfully that a mentoring relationship is not working for you.
If you have any concerns you may wish to share them with your tutor or your line manager.
Top Tip 4: Where and how will you meet?
You could meet face-to-face, have phone conversations, or make use of virtual technologies like Skype or zoom. People will have personal preferences – one size doesn’t fit all. It can be useful to hold your initial meeting face-to-face if that’s possible. You don’t have to stick to the same method of meeting – you can change it about according to preference, and personal need (thinking of diary commitments and travel time for example).
Top Tip 5: Transfer learning across primary and acute care
It is important that those working in Primary Care and Acute Care have an understanding of how the different sectors work and operate with regards to mentoring and learning. They often work quite differently and, whilst you might not be looking to necessarily move from one to the other this contextual knowledge and understanding is professionally important.
This is especially valuable, in terms of systems and processes. Most organisations have some access to mentoring eg NHS England has a voluntary mentoring scheme and ‘General Practice Ready’ offers access to trained mentors and primary care has Buddying Peer mentoring, using a pool of trained mentors. Ask if your organisation has something similar.
Asking colleagues across specialties is a great way to shape mentoring and to find a fit for you. In acute care there may be mentors available at ward level.
Top tip 6: Psychological support
Learning and development is not always about imparting specific skills and knowledge: it is often about providing emotional and psychological support to people. As a mentor, be a role model by being genuine, by being approachable, showing interest, being available and being non-hierarchical in relationships with mentees.
Everybody has something to offer: see their talents. Use positive psychology and strengths-based motivation techniques (that is, focusing on what someone can do, rather on what they can’t). Remember what it is like not knowing something or being unable to fulfil a role. Walk a mile in someone’s moccasins: ’don't judge others. Work on the positives and support your colleagues and feedback positive behavioural characteristics that you see from the mentor or mentee.
Both the mentor and mentee benefit from having well-developed emotional intelligence.
By learning more about ourselves, challenging ourselves, and being honest about ourselves we can be better able to support our colleagues, our patients, and their families especially during difficult times.
Top Tip 7: Review your own skills
A mentoring relationship is based on effective communication. These skills are two-way and are also valuable skills in our work with colleagues and patients or system users. At any given time, it is worth using reflective practice to consider how well are we doing, for example, do I listen effectively or am I thinking of what I’m going to say and miss what’s being said? Communication is a skill just like any other, and as such needs the investment of time, and practice.
Important examples include:
Balancing advice with support as a mentor, know when to offer advice or opinion, providing space for the mentee to discover their own solutions.
Listening skills, it is important to be able to actively listen and to pay close attention to what people are saying. Make sure you are really listening to what someone is saying, not what you think they are saying. A simple way of showing that you are listening, and to check that you have understood them correctly, is to reflect back what the other person has said. You can do this by feeding back their own words to them, or by paraphrasing.
Questioning techniques: Know when to ask open and/or closed questions. An open question would be something like “What did you think of that book?” which requires a detailed answer, rather than something like “Did you enjoy that book?” which requires a yes/no answer. Use questions to clarify and confirm what you’ve heard through listening to your mentor/mentee.
Providing feedback, we need to recognise that feedback is vital both when somebody is successful at something, and when not ready or not yet able to do something. It is also vital to consider how feedback is delivered and for it to be given in a positive frame. Be constructive, and give praise where it is due.
Top Tip 8: Develop key qualities of a mentor and reverse mentor
Effective mentors develop and utilise a number of key qualities such as:
- Showing compassion and authenticity
- Being honest but diplomatic in communication
- Being inquisitive
- Demonstrating objectivity and fairness
- Showing a willingness to communicate what you know
- Bing prepared for conversations
- Being committed to the relationship
Top Tip 9: Share resources
Are there resources that could help the mentee? These could be organisational resources, learning resources, or it could be people who know about specific subjects or aspects of work. Pointing people in the right direction is a key feature of mentoring. You may not know everything yourself, but you can point people in the right direction.
Hopefully you will use the ambassadors’ network to see who you might want as a mentor or reverse mentor to support you in your career or aspects of your role.
Top Tip 10: Learn about different roles and portfolios
As we know the NHS is rapidly changing, with roles and functions moving and shaping all the time. Actively seek out mentors from different sectors and different clinical areas, depending on what you want to learn about and where you might see your career progress. Be proactive in seeking out a mentor who may serve you well.
Remember your mentor does not always have to be a nurse, or a nurse in your field. The Ambassadors programme offers diverse opportunities for learning and sharing!
We give you permission to look wider and further to find a mentor that suits you.
Developing the Top Ten Tips
The Top Ten Tips were devised through a process of consultation with a number of people engaged in the Ambassadors programme. The themes presented below were derived from that consultation and have informed the Top Ten Tips together with other material outlining key features of effective mentoring programmes and positive mentoring relationships.
Those consulted were asked what goods mentors do, what poor mentors do and what do mentors need now and in the future.
A list of bullet points from those discussions is presented below.
Good Mentors - themes
- Help change your thinking thus your feelings and therefore your behaviour by supporting you to find the answers to the problems and practice you are working on
- Find time for you
- Use positive psychology and strength-based motivation techniques
- Are genuine, not patronising as people see through that
- Are approachable, interested, non-hierarchical
- Create a sense of belonging, recognition, contact
- Have a “contract” with their mentored- outline what is expected from both parties
- Use principles of no such thing as failure, all is feedback
- GROW model is a good model for feedback- share and use it- write a how to guide
- Listen
- See talents in individual, everybody has something to offer
- Encourages self-belief
- Know what they are talking about and shares that in an empowering way
- Uses humour
- Develops even the least senior staff as well as senior
- Shares ideas on how to work round issues and problems
- Reverse mentors- meaning that asks younger and sometimes more junior staff for their help - especially in digital learning platforms/ presentation of material/ This helps younger staff to find ways to support others and adds to their self-belief and challenges hierarchies
- Be kind
- Mentor who connects with your own learning style and preferences, maybe an NLP window of the world? I.e. visual/ AD/ auditory
Poor mentors – themes
- Not interested
- Do not respect boundaries
- Condescending attitude
- Not clear about work of Ambassadors/ trust/team
- Bullying
- Hierarchical
- Are inconsistent, cancel meetings, fail to keep commitments
- Are disorganised
- Try and micro manage
- Do not support and do a lot of telling
Further reading:
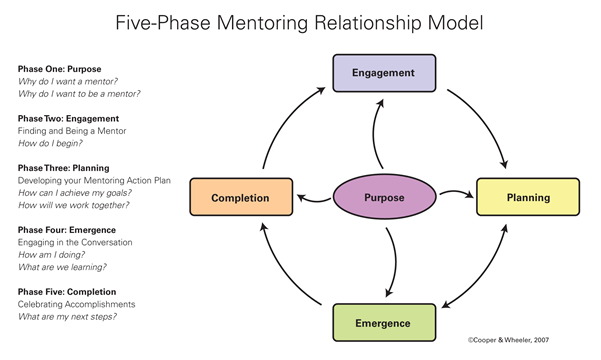
Mentoring Model – The Five-Phase Mentoring Relationship Model
The Five Phase Mentoring Relationship Model (MRM) developed by Mary Wheeler and Michelle Cooper has been used extensively with individuals and organisations as a framework for informal mentorship relationships and formal mentorship programmes.
A successful mentoring relationship is founded on mutual trust, shared values, interests, and commitment. Its success is largely dependent on the care taken to build it. The quality of the relationship has a significant effect on achieving mentoring outcomes.
Successful mentoring relationships require investing time to understand the why and the how of the mentoring relationship and commitment of time for ongoing focused interaction and reflection. Having a clear career goal that a mentor can help the mentee to achieve or that can be fulfilled by being a mentor is the first step in a successful mentoring relationship. Despite the significantly positive impacts and benefits that mentoring relationships can have, few know how to enter into and establish a mentoring relationship. Building a successful mentoring relationship is a learned skill that can be developed and sustained for both mentors and mentees.
Thank you to our contributors
The Ambassadors contributors who worked with Jude Goddard from Imagine Results to develop this resource were:
Andrea HargreavesMatron, University Hospital Coventry and Warwick NHS Trust
Dann Gooding, RCN representative and Student Nurse (Now Registered Nurse at Birmingham Childrens Hospital NHS Foundation Trust)
Joanne Mohammed, Sister, East Lancashire Hospitals NHS Trust
Patience Akiri, Royal National Orthopaedic Hospital NHS Trust
Zara Head, Lead Nurse, Doncaster Clinical Commissioning Group
Jo Hockley, Matron, Maidstone and Tunbridge Wells NHS Trust
Jemma Sharples, Learning Disability Nurse Advisor, NHS England
Karen Storey, Primary Care Nursing Lead, NHS England



/Passle/5a5c5fb12a1ea2042466f05f/MediaLibrary/Images/6168334917af5b10f4bf1d30/2022-04-14-15-27-52-040-62583d78f636e9115805b2d5.png)
/Passle/5a5c5fb12a1ea2042466f05f/MediaLibrary/Images/6168334917af5b10f4bf1d30/2022-08-05-09-59-36-465-62ecea08f636e906acfed639.jpg)
/Passle/5a5c5fb12a1ea2042466f05f/MediaLibrary/Images/6168334917af5b10f4bf1d30/2022-07-28-14-57-17-405-62e2a3cdf636e9180c9835cb.png)
/Passle/5a5c5fb12a1ea2042466f05f/MediaLibrary/Images/6168334917af5b10f4bf1d30/2022-07-20-10-16-56-533-62d7d618f636ea07987f6668.png)
/Passle/5a5c5fb12a1ea2042466f05f/MediaLibrary/Images/6168334917af5b10f4bf1d30/2022-07-15-09-55-32-858-62d13994f636ea1398e71aa9.jpg)